
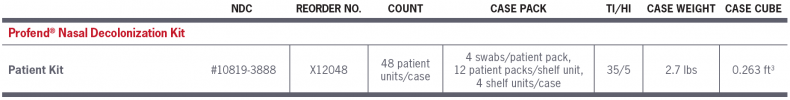
No single approach can fully eliminate the risk of healthcare-associated infections (HAIs). That’s why healthcare institutions need multiple layers of defense to attack infections from all angles. Profend® nasal decolonization kit can help provide effective infection risk reduction at the innermost layer: patients themselves. It’s just one of PDI Healthcare’s integrated products that helps you implement an overall infection prevention strategy.
Nasal decolonization with PVP-Iodine is now a CDC core strategy for reducing S. aureus in high-risk surgeries.5


References:
1. VandenBergh MF, Yzerman EP, van Belkum A, Boelens HA, Sijmons M, Verbrugh HA. Follow-up of Staphylococcus aureus nasal carriage after 8 years: redefining the persistent carrier state. J Clin Microbiol. 1999;37:3133–3140. 2. Septimus EJ. Nasal Decolonization: What antimicrobials are more effective prior to surgery? Am J Infect Control 2019;47S:A53-A57. doi: 10.1016/j.ajic.2019.02.028. 3. Kalmeijer MD, van Nieuwland-Bollen E, Bogaers-Hofman D, de Baere GA. Nasal carriage of Staphylococcus aureus is a major risk factor for surgical-site infections in orthopedic surgery. Infect Control Hosp Epidemiol. 2000;21(15)319-323. 4. Anderson DJ, Kaye KS, Chen LF, Schmader KE, Choi Y, et al. Clinical and Financial Outcomes Due to Methicillin Resistant Staphylococcus Aureus Surgical Site Infection: A Multi-Center Matched Outcomes Study. PLOS ONE. 2009;4(12):e8305. doi:10.1371/journal.pone.0008305. 5. Centers for Disease Control and Prevention. Strategies to Prevent Hospital-onset Staphylococcus aureus Bloodstream Infections in Acute Care Facilities. https://www.cdc.gov/hai/prevent/staph-prevention-strategies.html. Published December 2019. Accessed December 10, 2020. 7. Instructions for use. 8. PDI user acceptance study. 9. Maslow J, Hutzler L, Cuff G, Rosenberg A, Phillips M, Bosco J. Patient experience with mupirocin or povidone-iodine nasal decolonization. Orthopedics. 2014;37(6):e576–e581. 9. 1PDI in vivo Study 0113-CTEVO. 10. Citation: Sievert D. Antimicrobial-resistant pathogens associated with healthcare associated infections: summary of data reported to the NHSN at the CDC, 2009-2010. Infect Control Hosp Epidemiol. 2013;34(1):1–14. 11. Citation: https://www.cdc.gov/hai/data/portal/index.html 12. Citation: https://jamanetwork.com/journals/jama/article-abstract/2752664 13. PDI Study PDI-0113-KT1
*Surgical site infections
